Small, consistent changes can reduce falls, ease confusion, and keep daily life calmer. Use this walkthrough to tune each space—then review monthly as needs change.
|
Front Entry & Living Areas |
|
Goals: clear pathways, fewer tripping hazards, strong visual cues. |
|
Quick wins
Setups that help
Red flags
|
|
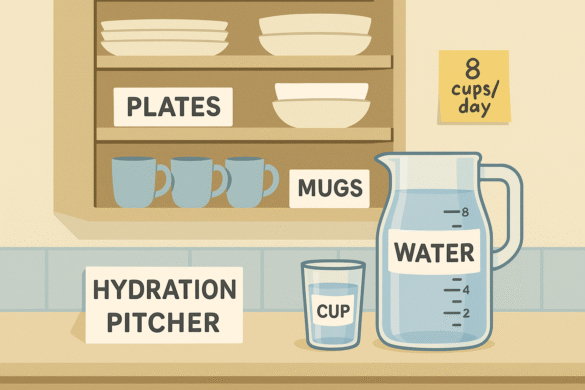
Kitchen |
| Goals: prevent burns/cuts, simplify choices, promote hydration and nutrition. |
|
Quick wins
Setups that help
Red flags
|
|
Bathroom |
| Goals: safe transfers, prevent slips, maintain dignity. |
|
Quick wins
Care tips
Red flags
|
|
Bedroom |
| Goals: good sleep cues, easy dressing, safe night mobility. |
|
Quick wins
Evening routine
Red flags
|
|
Hallways & Stairs |
| Goals: visibility, hand support, no tripping hazards. |
|
Quick wins
Red flags
|
|
Exits & Outdoors |
| Goals: safe entrances, planned activity, prevent unsafe wandering. |
|
Quick wins
Red flags
|
Whole-Home Systems (the glue that holds it together)
Labels & signage
-
Big-label room signs and drawer labels; simple words + icons.
Daily plan
-
Whiteboard with today’s plan: breakfast → walk → lunch → quiet time → dinner → bedtime.
Evening (sundowning buffer)
-
Lights on before dusk, curtains closed, familiar music, one simple task (fold towels).
Med & safety management
-
One pharmacy if possible; weekly organizer; RN teaching for new/complex meds.
-
Go-bag: med list, allergies, recent vitals, insurance cards, advance directives, key contacts.
Technology (optional)
-
Video doorbell, stove shutoff devices, motion sensors, location services if recommended.
© 2025 MedPro USA Health Services. All rights reserved.
Caregiver Notes (protect your energy)
-
Build two 15–20 minute breaks into each day (neighbor or sitter).
-
Hydration and a short walk for you count, too.
-
If safety worries are constant, you don’t have to carry it alone—ask for a home-health assessment.
When to Call for Clinical Help
-
Sudden change in behavior or confusion (possible infection, dehydration, pain, medication effect).
-
New or repeated falls, unsafe wandering, frequent nighttime wakefulness.
-
Weight loss, poor appetite, swallowing trouble, skin breakdown.
-
Caregiver exhaustion.
How we help: Our nurses, caregivers, and therapists assess risks, set up your safety plan, train family on transfers and calming techniques, coordinate with your physician, and help prevent avoidable ER visits.
Ready to make a plan?
Memorial & Greater Houston 📞 713-932-0017 • Info@MPUHealthServices.com
🏠Address: 9219 Katy Freeway, Suite 207, Houston, TX 77024 • Web: mpuhealthservices.com
Download: Dementia Home Safety — Quick Checklist (PDF)
Dementia Home Safety Checklist